Document process management frees up GP time
It’s well documented that general practice faces unprecedented challenges. As a result, probably more than at any other time in recent history, big changes are having to be made, causing plenty of headaches for clinicians and practice managers. Throw into the mix an evermore transparent world of reviews, inspections and public feedback and it means practices are having to get creative – not just to deliver core services but, crucially, to be constantly innovating and improving them. Quality Improvement (QI) has become a key focus.
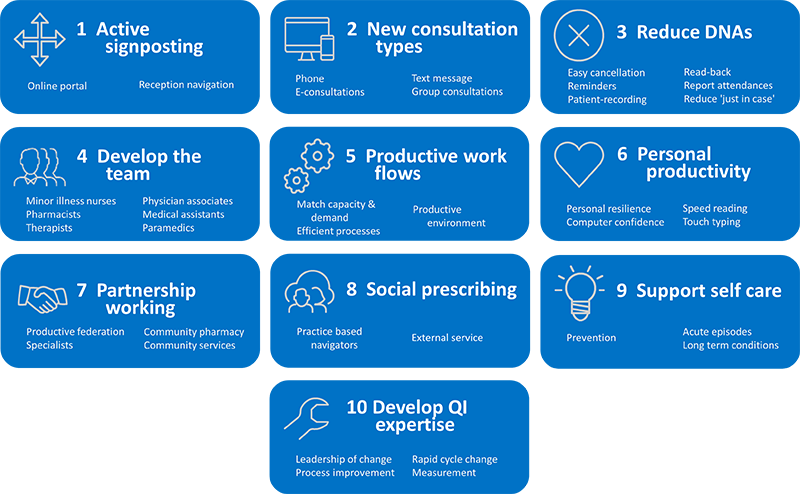
This is a topic that hasn’t gone unnoticed by the NHS. In its Releasing Capacity in General Practice initiative, the tenth High Impact Action listed is ‘Building QI Excellence’. In a nutshell, this is essentially about developing a specialist team of facilitators to support service redesign and continuous quality improvement.
The idea is that such a team will enable faster and more sustainable progress to be made on the other nine high impact changes. The team could be based in a CCG or federation. They should ideally include clinicians and managers, and have skills in leading change, using recognised improvement tools such as Lean, PDSA and SPC, and coaching GP practice teams.
Developing QI
Dr Robert Varnam, Head of General Practice Development at NHS England, writing on the NHS Networks site suggests practices have two ways to go about building QI:
Facilitated change: One popular approach to building your team’s capabilities for service redesign is to undertake a programme of change with external facilitation.
This approach to ‘learning while doing’ focuses chiefly on the change project, often addressing something like the appointments system or repeat prescription handling. External expertise is used to guide the planning and delivery, and they provide coaching for the team and leaders through the process. The secondary aim is to build confidence in using the relevant redesign methods, thus leaving a legacy of increased capability for the future.
It is worth taking care to choose an external coach or team who will help you address a high profile need in the practice as well as build your intrinsic capabilities for the future. Purchasing external support that does not leave a legacy can end up being very costly.
Capability building: Another approach is to focus chiefly on training and coaching to develop the awareness and skills of an individual of team. This provides them with a thorough understanding of a range of approaches to leading change, the reasons why they work and how to apply them in different situations.
For busy primary care staff it is usually best to apply a learn-while-doing approach to training like this, as few people are interested in committing to a more academic learning experience. Action learning with expert coaching and personal study can help develop capabilities for the future at the same time as accelerating the implementation of a live change project.
Practice success
Quality improvement comes in many different forms – it can cover any part of a practice’s processes or service delivery. One GP that has enjoyed success is Bridge House Medical Centre in Warwickshire, a practice with over 9,000 registered patients where GPs have enjoyed an 83 per cent reduction in dealing with incoming paperwork. Their story has featured in an NHS case study.
The practice, along with a group of 13 other practices within South Warwickshire, took part in Learning in Action, a collaborative approach to learning and improvement. Among the areas the group selected to focus on improving was document management, giving the practice an opportunity to look at how to introduce new ways of working involving training administrative staff to deal with clinical administration tasks.
Gradual development
Using the Plan, Do, Study, Act cycle – more information can be found here – the practice carried out a small test cycle with a Standard Operating Procedure. The procedure set out the types of correspondence the GPs received and what they did and did not need to see each day. The test involved admin staff and the practice manager working through the previous month’s letters to see what actions they would take following the Standard Operating Procedure. The results showed that 20% of the correspondence did not need to be sent to the GPs.
The second cycle was on the ability to develop a pathway for certain types of letters, ensuring there is an agreed set of principles and a standard approach for the process. The first pathway tested was on diabetic eye screening letters, where there was frustration from the CCG around the level of coding with regard to retinopathy screening. To improve this, ensure the data was visible in the patient record, and some enhanced steps to the actions taken on receipt of these results, the practice carried out a process mapping exercise during one of the workshops. One of the outputs was to develop and test a template to match the format of the hospital letter and a pathway written.
Supporting staff in change
The aims and objectives of the project were discussed with the whole practice team and role changes with individual members of staff were discussed during appraisals. The clinical team was involved in the process including a GP processing all of the documents for one week to see what was coming in, how much work it involved and how the process could be managed better.
A Standard Operating Procedure was developed with all clinicians for a consistent approach to what documents they still needed to see. One receptionist and one member of the admin team underwent the practice’s training programme, mentored by the practice manager, and also took part in training events organised by the federation.
Sharing and learning with other practices
The Learning in Action workshops enabled the practice time to think and share ideas. Breaking the process down into small steps made it easier to start the change process and identify weak spots the practice was able to adjust accordingly. For example, demonstrating ‘safety’ in the new method was worked through during shared discussions, where the practice found it could build into the audit the review of ‘safety’.
Measurement was also discussed and the practice was able to break down and identify a baseline measure.
The main impacts of the programme are:
- The volume of incoming paperwork going to GPs has reduced by 83 per cent per week, collectively releasing seven hours of GP time a week.
- GPs can now spend more time on the correspondence they receive and the actions highlighted for them e.g. on reading one letter to the end a GP discovered that the list of current medications on page one had in fact been stopped and replaced with another. He felt he may not have had time to spot this had he been working through 60 or 70 letters rather than the 8 letters he had that day.
- Staff are very positive and the two team members taking on the role are very enthusiastic.
- The change of role offered ensured the practice was able to retain one team member who without this opportunity for development would have left the practice.
- Other members of the reception team who no longer have to code letters were trained on active signposting.
Commenting on the initiative, Marie Tew, Practice Manager at the Bridge House Medical Centre said: “A lot of the work we undertook in the planning stage we did at the Learning in Action workshops. Without the sharing and learning from other practices and protected time to consider the problems, we probably would never have got this going at all.”
The above is just one example of how practices are embracing QI with success and more can be found on NHS Networks. General practice is a process driven business – and as such there’s plenty of scope to use QI to help free up your time and deliver service excellence.
Have you found new ways of working in practice that you could share with us and other PMs? Join the discussion here




0 Comments